Understanding Why You Still Feel Tired On Thyroid Medication
Many patients expect an immediate resolution of fatigue after beginning prescription therapy, yet feeling exhausted is a persistent complaint. This often occurs because the goal of treatment is sometimes defined as getting test results into a standard reference range rather than ensuring symptom relief. A patient might see their numbers move into the "normal" category while still struggling to get out of bed in the morning.
Understanding why you still feel tired on thyroid medication requires looking beyond basic reference ranges. Standard lab ranges are broad and designed to diagnose disease, not necessarily to optimize health for every individual.
Common misconceptions regarding thyroid health include:
- Confusing "Normal" with Optimal: A result within the reference range does not guarantee the absence of symptoms.
- Over-reliance on TSH: Thyroid Stimulating Hormone (TSH) is a pituitary hormone, not a direct measure of active thyroid hormones available to your cells.
- Ignoring T4 and T3: Focusing solely on TSH misses the conversion process where the body must turn storage hormone (T4) into active hormone (T3).
Relying on TSH levels alone may not reflect your actual energy status because TSH can lag behind changes in tissue metabolism. Comprehensive testing often reveals that while TSH looks acceptable, levels of Free T3 may be suboptimal, leaving you without the energy needed for daily activities.
Inadequate Dosage and Absorption Issues
One primary reason you might wonder why you still feel tired on thyroid medication is that your prescribed dosage of levothyroxine is simply insufficient for your body's specific needs. A dosage that effectively normalizes blood test results may not completely alleviate symptoms for every patient, leaving you with lingering fatigue. Common signs that your current dosage is too low include persistent exhaustion, unexplained weight gain, dry skin, and an inability to tolerate cold temperatures.
Even with the correct dosage, poor absorption can prevent the medication from working effectively. Timing significantly influences how well the body utilizes the drug. Levothyroxine must be taken on an empty stomach, ideally in the morning, at least 30 to 60 minutes before breakfast. Consuming food or coffee too soon can drastically reduce the amount of hormone absorbed into the bloodstream.
Furthermore, interactions with common supplements can interfere with treatment. Many patients take vitamins or minerals that inadvertently block thyroid medication absorption. To avoid this issue:
- Take calcium supplements at least 4 hours apart from your thyroid medication.
- Separate iron tablets and multivitamins containing iron by a similar 4-hour window.
- Avoid taking fiber supplements or soy products simultaneously with your dose.
The Role of Nutrient Deficiencies in Fatigue
Persistent exhaustion despite taking thyroid medication often stems from underlying nutrient gaps. Low iron or ferritin levels are a primary culprit, as iron is essential for transporting oxygen to cells. Even without full-blown anemia, depleted ferritin stores can leave you feeling weak and breathless, directly mimicking thyroid-related fatigue.
Vitamin D and B12 are equally critical for optimal thyroid function. Vitamin D acts as a key modulator for the immune system and aids in converting thyroid hormones into active forms. Meanwhile, Vitamin B12 is necessary for energy production at a cellular level; a deficiency can cause neurological symptoms and severe lethargy that medication alone cannot fix. For example, a patient might normalize their TSH levels but still struggle to get out of bed if these co-factors are missing.
Standard thyroid panels often miss these hidden deficiencies. To truly understand why you still feel tired on thyroid medication, comprehensive testing is required. This should go beyond TSH and T4 to include:
- Ferritin: Measures stored iron, not just circulating levels.
- Vitamin D (25-OH): Assesses total storage levels of the vitamin.
- Vitamin B12: Determines if levels are sufficient for red blood cell formation and energy.
- Magnesium and Zinc: Additional co-factors that support hormone synthesis and utilization.
Addressing these specific deficiencies is frequently the missing link in restoring vitality.
Unlock Your Thyroid Energy
Support T4 to T3 conversion and restore balance with Thyrafemme. Go beyond normal ranges and feel truly energized.
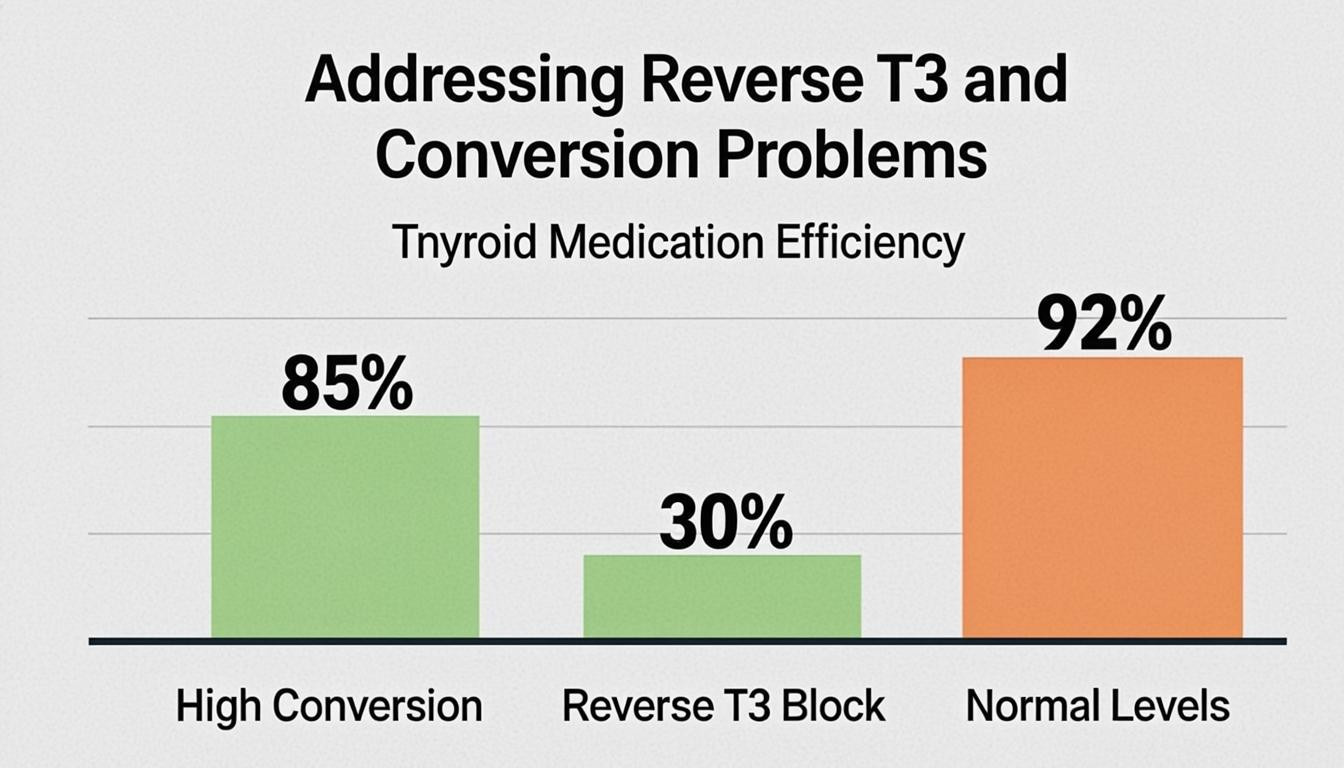
Addressing Reverse T3 and Conversion Problems
Reverse T3 (rT3) is an inactive metabolite of thyroxine (T4) that structurally resembles active triiodothyronine (T3). When rT3 levels rise, it competes with T3 for cellular receptor sites. However, unlike T3, rT3 binds to these receptors without activating them, effectively blocking active thyroid hormone from entering your cells. This creates a functional state of hypothyroidism at the tissue level, even if standard blood tests appear normal.
Chronic stress significantly disrupts the thyroid conversion process. High cortisol levels, often resulting from prolonged stress, inhibit the enzyme responsible for converting T4 into active T3. Instead, the body shunts T4 toward the production of reverse T3 as a protective mechanism to slow down metabolism. Consequently, this physiological response is a primary reason why you still feel tired on thyroid medication.
Prescribing T4-only medication, such as levothyroxine, may not resolve fatigue if the body cannot efficiently convert that hormone into T3. Factors contributing to poor conversion include:
- Chronic inflammation
- Nutrient deficiencies like selenium or zinc
- Severe calorie restriction
- Unmanaged stress
For patients struggling with persistent exhaustion, evaluating rT3 levels and cortisol balance is often necessary to optimize treatment.
Lifestyle Factors Influencing Thyroid Health
Understanding why you still feel tired on thyroid medication often requires examining daily habits. Sleep quality directly impacts thyroid regulation, as the majority of thyroid hormone secretion occurs during nocturnal rest. Poor sleep patterns can disrupt circadian rhythms, leading to imbalanced hormone levels and persistent fatigue.
Diet and blood sugar stability are equally critical. Fluctuating glucose levels force the body to work harder, draining energy reserves that are already low in thyroid patients.
To support energy levels, focus on the following dietary strategies:
- Eat balanced meals containing protein, healthy fats, and fiber to prevent glucose spikes.
- Avoid excessive caffeine or sugar, which can lead to energy crashes later in the day.
- Choose nutrient-dense whole foods like vegetables, nuts, and lean proteins.
Exercise helps manage fatigue, but overexertion can backfire. Gentle movement stimulates metabolism without exhausting the body. Low-impact activities such as walking, yoga, or swimming allow patients to build endurance safely. Listening to physical limits ensures that exercise restores energy rather than depleting it further.
When to Re-evaluate Your Treatment Plan
If you are asking yourself why you still feel tired on thyroid medication, it may be time to reassess your current strategy. Persistent fatigue often indicates that your hormone levels are not optimized or that your body is not converting the standard T4 medication into active T3 effectively. To address this, begin by keeping a detailed daily log of specific symptoms such as energy crashes, brain fog, and temperature sensitivity. Objective data provides a clearer picture for your provider during consultations.
Exploring combination therapy can be a necessary step for patients who do not find relief on T4-only monotherapy. This approach utilizes both Levothyroxine (T4) and Liothyronine (T3) to mimic natural hormone production more closely. Many individuals report improved vitality and metabolic function when T3 is added to their regimen.
Regular monitoring is crucial for long-term success. Thyroid needs can fluctuate due to stress, weight changes, or seasonal shifts. Adhering to a schedule of blood tests and dosage adjustments ensures your treatment evolves with your body's requirements.
- Track: Record daily energy levels and sleep quality.
- Discuss: Ask about T3 options if symptoms persist.
- Test: Schedule follow-up labs every 6 to 12 weeks initially.



Comments
0